MKSAP Quiz: Evaluation for progressive chest pain
A 56-year-old man is evaluated in the emergency department for progressive chest pain and dyspnea that began 3 hours ago. Medical history is significant for hypertension treated with lisinopril.
On physical examination, he is confused. Temperature is normal, blood pressure is 86/50 mm Hg, pulse rate is 118/min, and respiration rate is 24/min. Oxygen saturation breathing ambient air is 90%. Cardiac examination reveals an S3 gallop. Crackles are noted on pulmonary examination. The extremities are cool to the touch.
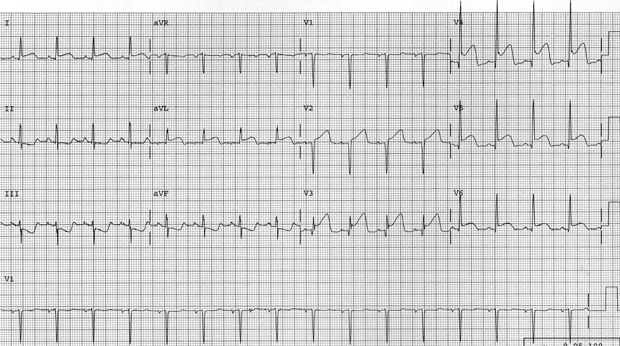
An electrocardiogram is shown. A chest radiograph reveals pulmonary edema.
Aspirin is initiated in the emergency department.
Which of the following is the most appropriate immediate management?
A. Admission to the ICU for medical stabilization
B. Intravenous metoprolol
C. Percutaneous coronary intervention
D. Sublingual nitroglycerin
E. Thrombolytic therapy
Answer and critique
The correct answer is C. Percutaneous coronary intervention. This item is Question 56 in MKSAP 18's Cardiovascular Medicine section.
Immediate percutaneous coronary intervention (PCI) is indicated in this patient with ST-elevation myocardial infarction (STEMI) complicated by cardiogenic shock. Cardiogenic shock is defined by persistent symptomatic hypotension and end-organ dysfunction. Patients have acute kidney failure, evidence of liver dysfunction with elevated aminotransferase levels, poor peripheral perfusion with cool extremities, and decreased mental status. Cardiogenic shock typically occurs as a consequence of a large anterior myocardial infarction, resulting in severely reduced left ventricular systolic function; it carries a mortality rate between 50% and 80%. Despite their instability, patients with cardiogenic shock (particularly those younger than 75 years of age) have a higher rate of survival if they undergo emergent revascularization with primary PCI in the catheterization laboratory.
Medical stabilization with intravenous vasoactive medications and, in severe cases, device-based hemodynamic support without prompt revascularization has been shown to be inferior to revascularization in the setting of shock and is not appropriate.
In the treatment of STEMI, β-blockers are recommended at the time of initial presentation, except in patients with evidence of hypotension, cardiogenic shock, pulmonary congestion, advanced atrioventricular block, or other contraindications to β-blocker therapy. Intravenous metoprolol is the most widely used β-blocker for STEMI treatment. In this case, β-blockade should be withheld and introduced following reperfusion therapy.
Intravenous nitroglycerin can be used to treat patients with STEMI and hypertension or heart failure but should be avoided in the setting of systolic blood pressure less than 90 mm Hg, significant bradycardia or tachycardia, right ventricular infarction, or use of a phosphodiesterase inhibitor (such as sildenafil) in the past 24 to 48 hours.
Because the rates of achieving vessel patency are higher and more reliable with primary PCI than with thrombolysis, primary PCI is the preferred method of treating STEMI. Thrombolytic therapy would be indicated in this patient with STEMI if transfer to a PCI-capable center would result in a first medical contact–to–device time of more than 120 minutes.
Key Point
- Patients with ST-elevation myocardial infarction complicated by cardiogenic shock should undergo emergent revascularization with primary percutaneous coronary intervention.



