MKSAP Quiz: Gradually progressive dyspnea
A 74-year-old man is evaluated for a 5-year history of gradually progressive dyspnea and dry cough without wheezing or hemoptysis. For the past 2 years he has had pain and occasional swelling in both knees. He has not had fever or lost weight. He smoked one pack of cigarettes a day from the age of 18 to 60 years. He worked as an insulator for 40 years.
Physical examination shows no digital clubbing or cyanosis. Auscultation of the lungs reveals bilateral end-inspiratory crackles.
Pulmonary function testing shows:
| Total lung capacity: | 67% of predicted |
| Residual volume: | 72% of predicted |
| FVC: | 65% of predicted |
| FEV1: | 75% of predicted |
| FEV1/FVC ratio: | 89% |
| Dlco: | 52% of predicted |
His chest radiograph is shown.
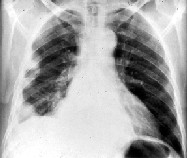
Which of the following is the most likely diagnosis?
A. Asbestosis
B. Idiopathic pulmonary fibrosis
C. Rheumatoid interstitial lung disease
D. Pulmonary sarcoidosis
Answer and critique
The correct answer is A: Asbestosis. This question can be found in MKSAP 15 in the Pulmonology section, item 12.
The diagnosis of asbestosis is based on a convincing history of asbestos exposure with an appropriately long latent period (10 to 15 years) and definite evidence of interstitial fibrosis without other likely causes. This patient worked as an insulator when asbestos exposure was still widespread and is at risk for asbestos-related lung disease. The most specific finding on chest radiograph is bilateral partially calcified pleural plaques. Pleural plaques are focal, often partially calcified, fibrous tissue collections on the parietal pleura and are considered a marker of asbestos exposure.
Rheumatoid lung disease has many manifestations, including an interstitial lung disease, which is most common in patients with severe rheumatoid arthritis. This patient's occasional swelling in both knees is not compatible with the diagnosis of rheumatoid arthritis.
Sarcoidosis occurs most commonly in young and middle-aged adults, with a peak incidence in the third decade. More than 90% of patients with sarcoidosis have lung involvement. The chest radiograph may show hilar lymphadenopathy alone, hilar lymphadenopathy and reticular opacities predominantly in the upper lung zone, or reticular opacities without hilar lymphadenopathy. Pulmonary function tests may reveal a restrictive pattern and reduction in Dlco, or may be normal. The patient's age, predominantly lower lobe involvement, occupational history, and pleural plaques argue against pulmonary sarcoidosis.
Idiopathic pulmonary fibrosis presents with slowly progressive dyspnea and a chronic, nonproductive cough. The chest radiograph is almost always abnormal at the time of presentation, with decreased lung volumes and basal reticular opacities. Almost all patients have a physiologic restrictive process (decreased forced vital capacity, total lung capacity, functional residual capacity) as well as impaired gas exchange with a decreased Dlco. However, asbestosis is a much more likely diagnosis in a patient with a positive exposure history and radiographic evidence of pleural plaques.
Key Point
- Pleural plaques are focal, often partially calcified, fibrous tissue collections on the parietal pleura and are a marker of asbestos exposure.